When you come down with an illness—a fever or the flu, for instance—you may notice a strange smell setting onto your blankets and clothes. Even when you’ve recovered, the smell may still linger until you’ve thoroughly washed it away. Many people know the odor that often accompanies illness as the “smell of sickness”; however, it is not the illness itself but rather the activated immune response that causes this “sick” smell. The ability to detect when others or themselves are ill are evolutionary skills to self-preserve the individual and the population. Depending on the illness, different immune responses may secrete smells that are unique from other illnesses. In ancient medicine, diagnoses were often made based on the immune system’s specific taste and smell. Even in more modern times, people have reported oddly specific smells to different kinds of illness: yellow fever smells like a butcher’s shop, typhoid like baked bread, and diabetes like rotten apples.
However, it is not the actual sickness, such as a virus or bacteria, that causes the odor. Even if an individual is not combating illness, they will still secrete the odor if their immune system were to be activated. In a 2014 study, researchers tested for actual distinguishable smells by giving participants 18 odor stimuli. To simulate an active immune response, they injected some healthy participants with an endotoxin, or lipopolysaccharide (LPS). LPS activates the cell’s toll-like receptors (TLRs), which triggers an active immune response as would naturally happen upon the invasion of bacteria or virus. This immune response may include releasing cytokines that cause inflammation and upregulating the molecules on antigen-presenting cells to maximize the effect of activating signals for attacking immune cells. The researchers used the shirts that the participants were wearing for the study. They sampled LPS body odors, placebo body odors, and control samples from unworn t-shirts, for their participants to smell and describe using a scale for the intensity and pleasantness or aversion for the smelling samples. The study showed that participants were able to distinguish an immune-response smell. The immune-response samples were also higher on the intensity and unpleasantness scales than placebo and control samples. Though the participants with the LPS body odors did not actually have an illness that would naturally cause the active immune response, their body upon artificially-created immune activity still secreted the unpleasant smell. This may be because the inflamed immune system either secretes a completely different smell than the immune system of a healthy person usually does, or secretes the same odors at a higher intensity.
A study published in 2015 found that gonorrhea, an STD caused by a specific species of bacteria, could also be correlated with an unpleasant odor. This study used the sweat of male participants, either both with, without, or recovered from gonorrhea, and tested whether young women were able to distinguish the health statuses of the tested sweat sample. The study concentrated on the presence of immunoglobulin A and G, IgA and IgG respectively, which are antibodies produced by the body to fight bacterial infection. This determines how high of an immune response the otherwise healthy male participants had, which indicates how healthy they were. For instance, the participants with higher concentrations of IgA and IgG, as determined from their saliva samples, would likely have a less healthy body at the time, such as a gonorrhea infection. The study found that the participants smelling the sweat samples associated a putrid scent to the sweat samples of the participants with gonorrhea, while the control and recovered samples that did not have gonorrhea had a more pleasant odor. Not only does immune response odor indicate sickness so that others might avoid catching the same illness, but it also very likely plays a role in reproductive selection. Individuals with a more putrid odor, such as in those who carry an illness, could decrease the odor attractiveness that the individual has to a potential partner.
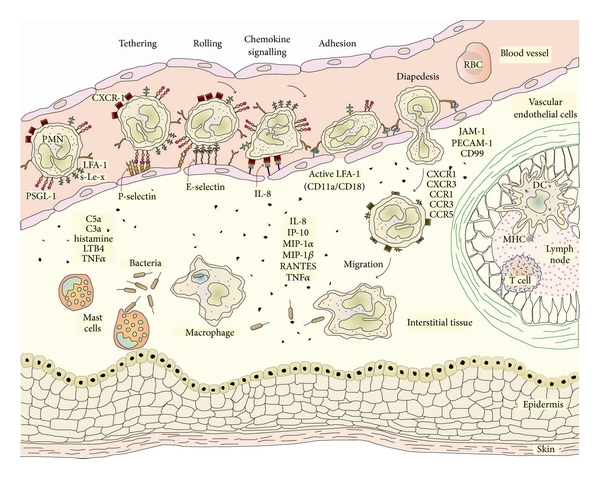
Another study discovered that body odors during illness may differ if the body has been infected by different bacteria. The study used mice samples and measured smells in their volatile body odors, which is based on the common odor compounds that are present in normal secretion. Mice were treated with different chemicals, one group with a mixture of LPS and phosphate-buffered saline solution (PBS), and another with only PBS for the control. The study collected urine samples from the mice with different inflamed immune systems, thus secreting different odors, and used six biosensors to attempt to distinguish between the urine samples. The study’s first two trials showed that both machines and mice were able to distinguish a presence or lack of inflamed immune response based solely on odor. The next trials now included urine samples from mice with different injections to simulate different immune responses. These immune responses mimic the immune response to different illnesses. The biosensors were able to predict different urine scents from mice treated with different injections. The mice were also able to distinguish a difference between those treated with LPS from those treated with different injections.
Understanding the difference between a normal body odor and the odors caused by an inflamed immune system can help protect yourself and others. If further studied and innovated upon, this evolutionary response can potentially be used to create an efficient diagnostic tool for medical professionals.
Sources:
- https://journals.sagepub.com/doi/full/10.1177/0956797613515681
- https://www.nationalgeographic.com/science/article/smell-sickness-parkinsons-disease-health-science#:~:text=Scientists%20have%20found%20that%20dozens,if%20you%20can%20imagine%20that.
- https://pubmed.ncbi.nlm.nih.gov/24452606/#:~:text=This%20chemosensory%20detection%20of%20the,altering%20patterns%20of%20interpersonal%20contact
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3549535/#:~:text=Lipopolysaccharide%20(LPS)%20is%20a%20natural,molecules%20on%20antigen%20presenting%20cells.
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3459149/#:~:text=Co%2Dstimulatory%20molecules%20are%20a,influencing%20T%20cell%20differentiation%20and
- https://www.sciencedirect.com/science/article/abs/pii/S1743609515338133?via%3Dihub
- https://www.cdc.gov/std/gonorrhea/stdfact-gonorrhea-detailed.htm#:~:text=Gonorrhea%20is%20a%20sexually%20transmitted,with%20the%20Neisseria%20gonorrhoeae%20bacterium.
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8286090/

