The coronavirus pandemic triggered a rise in the general public’s interest in the world of pharmaceuticals. Curiosity regarding the development and production of drugs by companies like Pfizer and Moderna has become a centerpiece of everyday conversation in the past three years. How does the COVID-19 vaccine work? How was it created, and how was it tested before being approved for public use? In order to really understand the biology behind the coronavirus vaccine and other drugs so common to us, we need to go all the way back to the mid-nineteenth century.
Paul Ehrlich, a German scientist and physician, worked in his cousin’s stain and dye lab. There, he made the seemingly small but vital discovery that certain dyes color only a specific organ, tissue, or cell in the body via tissue sample staining. These studies of dye selectivity led Ehrlich to theorize the existence of what he called “magic bullets,” or molecules that are able to selectively target specific parts of the body via cell receptors. Using both his medical knowledge and previous experience with dyes, Ehrlich began to research magic bullets with potential medicinal properties against bacteria and parasites. He uncovered that a dye named methylene blue not only has a particular affinity for staining parasites and bacteria, but it also is able to kill a parasite common to the tropical regions of the world known as malaria. These results were confirmed when Ehrlich ran a two-patient clinical trial in which a methylene blue treatment was able to break both of the participants’ malaria-induced fevers and clear their bloodstreams of the parasite with very few negative side effects. Due to not having access to a large number of malaria patients, Ehrlich was unable to continue his studies on methylene blue as a magic bullet. However, he continued to develop selective medications throughout his career—-for example, he discovered arsphenamine, the first effective treatment against syphilis—before passing away in 1915.
The concept of the magic bullet is the foundation of the modern pharmaceutical industry because all of today’s medications are selective. For example, one of the most common over-the-counter medications today is Advil, which contains ibuprofen to ease pain. Ibuprofen is a “magic bullet” because it is designed to recognize and attach only to pain receptors throughout the body. Once bound to these receptors, it is able to begin the chemical reactions necessary to ease one’s pain. Ehrlich’s “magic bullet” is truly the magic behind modern medication.
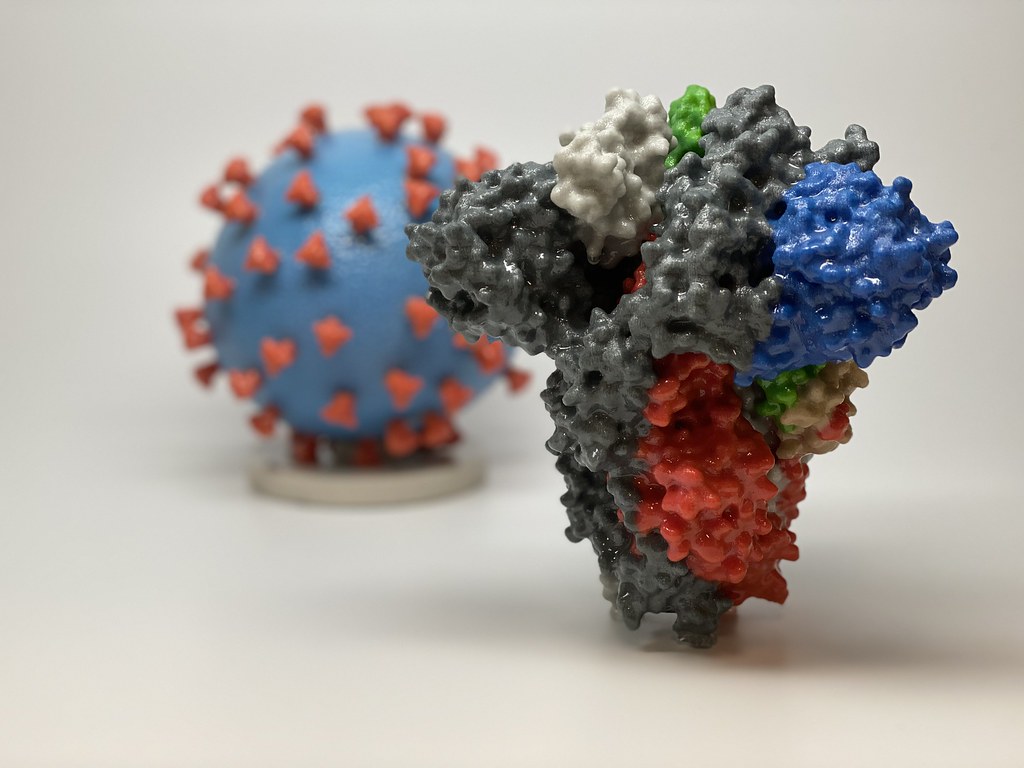
The most recent pharmaceutical innovation was the development of the coronavirus vaccine in mid-2020. Similar to methylene blue and Advil, the vaccine allows the body to selectively attack what is causing it harm. For example, when the Pfizer mRNA—a type of RNA (ribonucleic acid) that carries genetic information from the DNA to the ribosomes in order to synthesize proteins—vaccine is injected into someone, it enters their muscle cells and produces a molecule found on the surface of the coronavirus called spike protein. Once these proteins are created, they stay on the surface of cells and are recognized by the body as abnormal. This triggers an immune response within the body to fight off the supposed “infection.” During the immune response, white blood cells known as B-lymphocytes create monoclonal antibodies (mAbs) specific to the coronavirus. These antibodies are able to bind to the virus, thus causing other immune white blood cells, like macrophages, to attack and destroy it. Once this has occurred, the response is stored in the body’s memory, specifically the antibodies’ memory, and it will automatically begin at a faster rate when future spike proteins are detected. Thus, the mRNA vaccine operates on similar principles to Ehrlich’s “magic bullet” as it allows the body to selectively recognize and attack the COVID-19 virus.
Similar to methylene blue, the coronavirus vaccine also underwent a clinical trial to ensure its efficacy, except it was much more extensive than that of methylene blue. While the methylene blue trials only had two participants, Pfizer’s coronavirus trials had 46,331. Additionally, Ehrlich did not make use of any controls in his trial while Pfizer used a placebo, a vaccine with no effect on patients, in order to ensure that the participants that received the actual vaccine were protected from COVID. Overall, the Pfizer trial was much more effective than Ehrlich’s. While his trial did show positive results, he simply did not have enough data to definitely conclude that methylene blue is a reliable medication against malaria. The differences in these two clinical trials can be explained by the times in which they took place. Modern clinical trials are much more regulated and have much more resources available to them than those conducted back in Ehrlich’s time.
Paul Ehrlich has been named the father of modern pharmaceuticals because his concept of the “magic bullet” perfectly explains how modern drugs work in our bodies. While the development and testing of medication are much more advanced today, as shown by our much more thorough clinical trials, it is still rooted in the science that was uncovered back in the mid-nineteenth century.
Sources:
- https://www.sciencehistory.org/historical-profile/paul-ehrlich
- https://www.nature.com/articles/nrd2582
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6738855/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2790789/
- https://www.hopkinsallchildrens.org/Patients-Families/Health-Library/HealthDocNew/How-Do-Pain-Relievers-Work
- https://www.cdc.gov/coronavirus/2019-ncov/vaccines/different-vaccines/how-they-work.html
- https://www.ncbi.nlm.nih.gov/books/NBK279364/
- https://www.covid19treatmentguidelines.nih.gov/therapies/antivirals-including-antibody-products/anti-sars-cov-2-monoclonal-antibodies/
- https://www.pfizer.com/science/coronavirus/vaccine/about-our-landmark-trial