By Karen Tolentino | UTS Staff Writer | SQ Online (2014-15)

Dr. Anthony Cannella is an infectious disease specialist at the University of Florida whom I had the privilege of interviewing back in July. He attended the University of South Florida for his both his undergraduate degree and medical doctor (M.D.) degree. He has worked for UC San Diego Health Systems as a physician and a researcher.
Since the Ebola outbreak in West Africa, infectious diseases have begun to receive more attention around the world. According to the National Institute of Health (NIH), infection is the leading cause of death among the global population. Medical practitioners who pursue this specialty also work in internal medicine with an emphasis on the diagnosis and treatment of infectious disease. Becoming a specialist requires two to three more years of additional training after an initial seven or more years of medical school. During the interview, Dr. Cannella shared some of his thoughts on infectious disease and offered advice to students considering medical school.
- What interests you the most about infectious disease and why?
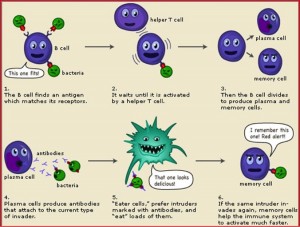
I find the human immune system fascinating. Every pathogen has different ways of attacking. Accordingly, the human body has developed ways to fight off these pathogens. This leads to the development of vaccines and toxins and allows for a huge range of variability between the attackers and the defenders. Our immune system is the first line of defense between us and the outside world, and without it we are very vulnerable. Infectious disease is really just a battlefield between the body and outside pathogens.
- Why did you decide to specialize in infectious disease?
I chose infectious disease because of its variety and dynamism. Infectious disease covers multiple parts of the body rather than just one part. It blends together internal medicine and microbiology and applies these fields to the pathology of processes taking place in the human body. When it comes down to it, organically, we are more bacteria and yeast than we are people. Our bodies are powered by interactions between microbes with generation times varying from 20 minutes to 24 hours. We share our bodies with other organisms and are completely dependent on them. For example, E. coli developing resistance to antibiotics leaves us vulnerable to illness. The microbiology aspect of infectious disease is always changing, always evolving, which keeps us on our toes.
- How does infectious disease interact with other specialties?
Sometimes, the spread of a disease can affect multiple parts of the body. In this case, we need to combine our knowledge of other organs in order to fully address the issue. This requires us working with specialists from other fields, such as cardiology and dermatology. This is how we gain insight into the disease and develop an appropriate diagnosis and course of treatment. As an infectious disease specialist, you have to gain an understanding of many different areas of the human body and collaborate across the board. This kind of work is extremely dynamic from a clinical and research perspective.
- What are your thoughts on the Ebola outbreak in West Africa?
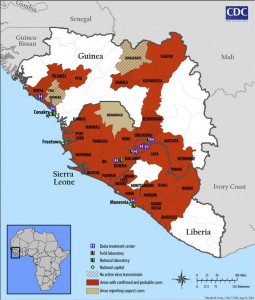
I think that the outbreak has received a lot of media attention because of the fear surrounding it. Ebola is associated with such dire symptoms, such as hemorrhaging all over the body and intense pain, that people have come to see it as an incredibly serious, frightening pathogen. There has been talk of it becoming an issue in the U.S. The fact of the matter is that Ebola would not have the same mortality rate in the U.S. as it would somewhere like West Africa. The mortality rates in either country would be much different. With our resources, we would have less of a problem keeping an outbreak under control in the U.S. as opposed to somewhere like Lagos, Nigeria. The aid workers in West Africa simply don’t have the resources available to effectively keep Ebola from spreading, and that is why such fear surrounds the outbreak. With the proper equipment, scientists, doctors and facilities, Ebola would be an easily containable infection. The affected countries are doing the best they can, but their economies have been ravaged by civil war and poverty. It’s up to larger countries, such as the U.S. and Europe, to decide whether they want to take a larger role in assisting countries fighting Ebola outbreaks.
- What advancements do you hope to see made in medicine, especially infectious disease, in the future?
First, I think we need to focus on improving antibiotics administered to fight infectious diseases. Lately, the development of such antibiotics has been stagnating. This has led to an epidemic of drug-resistant bacteria as existing antibiotics have begun to lose their effectiveness. Next, I think we should improve our understanding of the immune system to help develop new medications. One example I would give is the study of E. coli toxins. By understanding how these toxins impact the immune system, we can create a drug to bolster natural resistances against the toxins themselves.
- Do you have any advice for students thinking about medical school?
Reach out to those in the medical field and expose yourself to as many opportunities as possible. Don’t be afraid to put yourself out there and ask questions.
This concludes our interview with Dr. Anthony Cannella, Assistant Professor of Medicine at the University of South Florida. His unique perspective and insights into the medical field are much appreciated and hopefully provide food for thought for students considering medical school.
[hr gap=”0″]
Sources:
- http://www.nlm.nih.gov/medlineplus/infectiousdiseases.html
- http://www.ncbi.nlm.nih.gov/pubmed/25092109
- http://id.ucsd.edu/faculty/AnthonyCannellaMD-DivisionofInfectiousDiseasesUCSanDiego.shtml
- http://www.ajtmh.org/content/84/6/847.long
- http://www.theverge.com/2014/9/30/6875311/first-case-of-ebola-diagnosed-in-the-us-cdc-reports
- http://www.ncbi.nlm.nih.gov/pubmed/?term=Pathogenomic+Inference+of+Virulence-Associated+Genes+in+Leptospira+interrogans
- http://id.medicine.ufl.edu/sample-page/meet-the-team/anthony-p-cannella-m-d-m-sc/

