“My body, my choice”: A statement that demands autonomy over one of the only things that is truly ours in this world–our bodies. This very notion was challenged and struck by the law on June 24th, 2022 when the SCOTUS made a decision to overturn Roe v. Wade, enabling the criminalization of abortion on a state-by-state basis. Abortion has been a widely debated topic in politics and the media for many decades. Oftentimes, those who make the laws are not educated on the scientific background of abortions, creating a contorted web of challenges for the average woman to navigate alone.
Abortion is the deliberate termination of a pregnancy by medically removing the fetus from the uterus before it is able to survive independently. There are many reasons why someone may desire an abortion, such as complications with the mother or fetus’ health, financial instability, forced pregnancy as a result of rape/incest, an unwanted pregnancy, and more. No matter the reason for choosing to have an abortion, it should continue to be a medically safe and accessible procedure in healthcare. Outlawing abortion will not stop people from obtaining them, but it will increase the occurrence of unsafe abortions which can result in permanent disability, future infertility, risk of infection, and even death for the mother. Thus, criminalizing abortion is a misguided, unscientific insult to female reproductive rights.
To understand the importance of abortions in maternal health, one must first become familiar with how a fetus develops during pregnancy. To prepare for harboring a fetus, the mucous membrane lining the uterus, known as the endometrium, thickens in anticipation of fertilization. If fertilization does not occur, the endometrium lining is shed as part of the menstruation cycle. But when two haploid sex gametes (the egg and the sperm) fuse to give rise to a zygote, fertilization is successful. The zygote then undergoes a complex series of changes to become a self-sufficient, independent human. These changes occur in three main stages: the germinal stage, the embryonic period, and the fetal period.
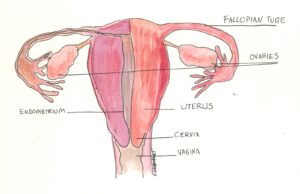
The germinal stage begins once the egg and sperm cell fuse their genetic material to form a zygote. The genetic makeup and sex of the zygote is determined at this point. A few hours after fertilization, the single-celled zygote journeys through the fallopian tubes (tubes connecting the ovary and the uterus) while exponentially replicating through a process of cell division called mitosis. Once the zygote grows to a size of eight cells, the cells start to differentiate and specialize to form organs and other unique body parts. At this point, the mass of cells is called a blastocyst. The growth rate of a blastocyst is rapid and exponential; by the time it reaches the uterus within only two weeks of fertilization, the single-celled zygote grows to upwards of 150 cells. The blastocyst then attaches to the wall of the uterus in a process known as implantation. If the blastocyst is unable to implant, it is expelled from the uterus during the next menstrual cycle. A serious complication that can occur at this stage is an ectopic pregnancy, which occurs when a blastocyst implants outside of the confines of the uterus, most often in the fallopian tubes. A fertilized egg cannot survive outside of the uterus, and when left untreated, an ectopic pregnancy can rupture the fallopian tubes and cause heavy internal bleeding. For the health and safety of the mother, this condition is treated with a medical abortion, either via surgery in extreme cases or medication in earlier stages. Without access to a safe abortion, the heavy internal bleeding and sudden abdominal pain caused by an ectopic pregnancy can be fatal. However, if the blastocyst successfully implants in the lining of the uterus, the menstrual cycle is halted by hormone signaling and the embryonic period begins.
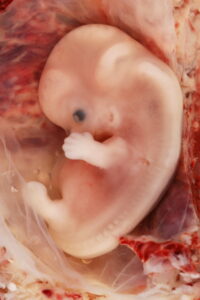
The embryonic period begins three weeks after fertilization and lasts until the eight week mark. In this period, the mass of cells, known as an embryo, develops into a blueprint of the human anatomy. Growing blood vessels form the placenta, which is attached to the wall of the uterus and connected to the embryo via a tube called the umbilical cord. The placenta provides oxygen and nutrients for the embryo while also acting as a garbage collector by filtering out carbon dioxide and harmful waste from the embryo. At approximately four weeks, the neural tube starts to form, which is a vital step as it acts as the embryonic brain and spinal cord. Complications with this developmental step can lead to devastating neural tube defects which occur when the tube doesn’t close properly. Examples include spina bifida–exposed spinal cord segments which cause motor, functional, and mental disabilities, and anencephaly–which occurs if the front part of the neural tube doesn’t close properly, resulting in the fetus being born without the forebrain (cerebrum). If a fetus with anencephaly is carried to term, it will likely be stillborn or survive for only a few hours after birth.

Following the formation of the neural tube, other parts of the body develop such as the head, nose, ears, eyes, mouth, limbs, and heart. At around six weeks, you can hear the heartbeat of the embryo, and by eight weeks the embryo has a completed blueprint of what it needs to become a fetus. When the basic structures of the brain and peripheral nervous systems are established and the production of neurons begins, the embryo can start to create a rudimentary neural network, which facilitates movement, development, and learning.
The fetal stage begins nine weeks after fertilization and ends at birth. At this stage, the blueprint of human anatomy develops into a semi-functional network of organ systems. Most lethal abnormalities in a fetus such as anencephaly or renal agenesis (absence of one or both kidneys) can be detected at 20 weeks. It may be favorable to opt for abortion in this case as the probability of life outside the womb for the fetus is almost none. Barring developmental issues, the neural tube develops into the brain and spinal cord, while neurons are engineered and deployed to specific sites in the body; connections between neurons are established and reflexes are developed. By the 24 week mark, the nervous system is completely established and the fetus can experience pain through sensations carried by neurons. This time also marks a significant milestone: the fetus has reached the age of viability. At this point, the fetus can survive outside of the womb with the help of ventilators, a sterile environment, and an intensive newborn care unit. Thus, most complications after this stage do not use abortions as medical treatment. From the 24th week until the 40th week, the fetus grows in size and function until it is born, ending the prenatal period and beginning life in the outside world.
It is integral to understand the science of prenatal development as it has a direct impact on women’s health. Pregnancy can be a grueling, challenging, and painful process for many and it must be a choice whether one wants to experience it. The mental and physical distress of a woman carrying an unwanted pregnancy can negatively affect the fetus’ physical and mental health to a great extent. There is evidence that a psychologically distressed pregnancy can result in long-term cognitive defects, behavioral problems, and high baseline levels of stress hormones once the fetus is born. Historically, abortion has been one of the most politically charged and divided topics in the United States, since the subject is deeply rooted in religious and ethical beliefs. Hence, understanding fetal development and abortion from a biological and psychological standpoint can be transformative in the way we administer prenatal care.
Sources:
https://www.verywellmind.com/stages-of-prenatal-development-2795073
https://www.health.com/news/abortion-medically-necessary
https://www.nbcboston.com/news/local/timeline-roe-v-wade-abortion-law-from-1973-2022/2755969/

