The human psyche is incredibly complex, so much so that we struggle to simply understand how the brain functions normally. Thus, you can imagine how hard it must be to try to make sense of brain activity resulting in abnormal behavior, such as mental illness. This struggle is apparent when we see how mental health was understood and treated throughout history. Even today, mental health-related medicine lags behind other areas, such as cardiovascular medicine. However, new breakthroughs in research suggest that precision medicine has the potential to significantly improve current diagnosing and treatment methods in psychiatry.
In the 18th century, mental illness was incredibly misunderstood. It was believed to be one of two things: demonic forces or physical illness. As a result, methods of treatment were, to put it lightly, horrendous. Examples include exorcisms, physical restraint and confinement in poorly maintained asylums, drilling holes in the skulls of patients (trephination), removing patients’ blood (bloodletting), and purging.
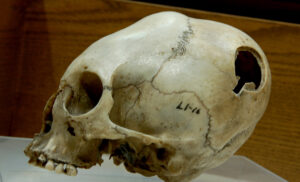
Image: Child’s trephined skull (Source)
Toward the end of the 19th century, our understanding of mental illness began to improve as two new psychiatric theories emerged: psychodynamic theory and the theory of behaviorism. Psychodynamic theory, proposed by Sigmund Freud, defined mental illness as the product of unresolved, unconscious motives. He suggested talk therapy as a form of treatment. On the other hand, John B. Watson believed that mental illness was related to behavioral conditioning, and thus, treatment should involve adaptive reconditioning—the use of stimuli to evoke and reinforce a desired response to a situation or an environment. These theories laid the framework for the development of modern pharmacological and psychotherapeutic approaches to psychiatric disorders in the mid-to-late 20th century, like cognitive behavioral therapy (CBT). CBT is a form of psychotherapy that aims to shift behavioral patterns by altering entrenched thinking patterns.
Despite the improvements that have been made in psychiatric medicine throughout history, current methods of diagnosing and treating mental health disorders are very random. While the Diagnostic and Statistical Manual of Mental Disorders provides a formal classification system for mental illness, so many disorders share similar symptoms that doctors have no choice other than to “guess and check” when diagnosing patients. This results in patients often being underdiagnosed or misdiagnosed. For example, bipolar disorder (BPD) is often underdiagnosed as depression. This is a problematic misdiagnosis leading to the wrong individuals getting prescribed prescription medications to treat depression. Incorrect prescriptions result in negative side effects such as further destabilization of mood, social and occupational impairments, substance abuse, depression, and suicidal ideation. Furthermore, even if a physician gets the correct diagnosis, each mental disorder has numerous potential treatments—counseling, dozens of prescription pills with differing dosages, brain stimulation therapies, support groups, etc.—which makes finding the best treatment (or combination of treatments) for a specific patient a very long, and sometimes difficult, process. Mental health treatment should not worsen an individual’s mental health. Fortunately, recent research shows that the path toward a more accurate diagnosis of mental disorders can be found in precision medicine.
Precision medicine is an approach to diagnosis and treatment for disease that aims to accurately diagnose illnesses, and optimize treatment benefits, and efficiency for a specific individual via genetic and molecular profiling. This approach is often used in cancer diagnosis and treatment. Biomarker testing (also known as tumor genetic testing, genome testing, molecular profiling, or somatic testing) provides valuable information about a patient’s cancer by looking for changes in specific genes and proteins. Different cancers produce unique changes, which are called biomarkers. Using biomarker testing, doctors are able to better select cancer treatments for patients because certain targeted therapies and immunotherapies only work for people with specific cancer biomarkers. For example, certain cancers are caused by changes in the EGFR gene—a gene that produces a protein involved in cell survival and growth. Biomarker testing would be able to indicate these changes in a patient, and as a result, their doctor would know to provide them with a treatment that would specifically target the EGFR gene.
In April 2021, Dr. Alexander B. Niculescu of the Indiana University School of Medicine published groundbreaking research regarding the use of precision medicine to diagnose and treat depression and mood disorders. In their study, Niculescu and his team tracked the high and low mood states of over 300 participants and noted the change in ribonucleic acid (RNA) biomarkers between these mood states. RNA’s one helical strand of bases plays a role in transforming the information stored in the genes of DNA into proteins that can carry out functions in the body. So, RNA biomarkers are RNA found in the bloodstream that indicate the presence of something abnormal in the body, such as disease. By comparing their findings with databases from previous studies, they identified 26 biomarkers that were present in participants with depression or mania, which are symptoms of mood disorders like BPD. From these findings, the team developed a blood test using these biomarkers to diagnose patients with either depression or a mood disorder and predict the risk of potentially developing one of these disorders in the future. Niculescu determined which biomarkers were targets of existing psychiatric drugs, thus allowing him to match patients to medication and measure their responses to the treatment.
Precision medicine has a strong promise for the advancement of psychiatric medicine. It will help distinguish between mental disorders with similar symptoms (e.g.depression and BPD) in order to avoid misdiagnosis and match patients with more effective treatments. Dr. Niculescu’s research is only the beginning of the progress that precision medicine will bring to the field of psychiatry. Recently, it has come to the attention of psychiatrists that attention-deficit/hyperactivity disorder (ADHD) is often misdiagnosed as anxiety. Similar blood tests to that developed by Niculescu could help in better distinguishing the two when doctors are trying to diagnose patients. The 19th century was a renaissance of sorts for psychiatry and mental health-related medicine, and with the rise of precision medicine, the 21st century might be one as well.
Works Cited:
- https://online.csp.edu/resources/article/history-of-mental-illness-treatment/
- https://bcmj.org/mds-be/historical-perspectives-theories-diagnosis-and-treatment-mental-illness
- https://healthitanalytics.com/news/blood-test-could-lead-to-precision-medicine-for-mood-disorders
- https://www.psychiatrist.com/jcp/bipolar/consequences-misdiagnosis-inaccurate-treatment-poor/
- https://www.fda.gov/medical-devices/in-vitro-diagnostics/precision-medicine
- https://www.cancer.org/treatment/treatments-and-side-effects/treatment-types/precision-medicine.html
- https://www.cancer.gov/about-cancer/treatment/types/biomarker-testing-cancer-treatment#what-is-biomarker-testing-for-cancer-treatment
- https://www.cancer.gov/publications/dictionaries/cancer-terms/def/egfr-gene
- https://www.nature.com/articles/s41380-021-01061-w
- https://www.healthline.com/health/adult-adhd
