BY LAUREN BRUMAGE | SQ ONLINE WRITER | SQ ONLINE (2017-18)
Public health officials are investigating a medical mystery that has spanned nearly two decades in Auburn, Alabama and Huntersville, North Carolina. Over 50 people in the two cities have been diagnosed with ocular melanoma, a rare form of eye cancer, since 1999 [1, 2]. Most of the patients are former students of Auburn University who attended the school from 1983 to 2001 [1, 2]. Ocular melanoma ordinarily has an incidence of 6 cases per 1 million people, so the diagnosis of at least 50 cases in just two locations is exceedingly unusual [1, 2]. While it seems that there may be a connection between the cases based on the narrow geographic scope, the cause of the cancer in these patients is yet to be determined.
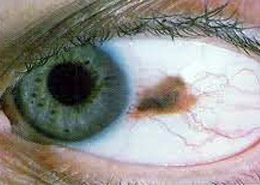
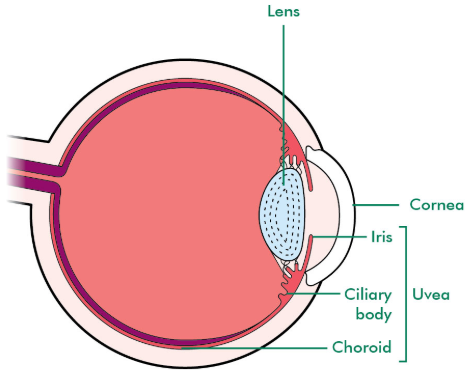
Ocular melanoma is cancer of the melanocytes, or pigment-producing cells, of the eye [3]. While the cause of ocular melanoma is still unknown, researchers do know that certain factors such as light-colored eyes, excessive UV radiation exposure, and/or having a mole on the eye can increase the risk of this form of cancer [3]. Most of those impacted tend to be 55 or older, rendering the Auburn-Huntersville group of cases all the more unusual as many in that group have been diagnosed in their 20s and 30s [1, 2, 4]. Women are also disproportionately represented in the Auburn-Huntersville ocular melanoma patient population [5]. The American Academy of Ophthalmology indicates that symptoms vary and can include vision abnormalities, flashes in vision, and spots on the eyes [6]. These same symptoms can also be caused by other eye conditions and may not always be obvious, making diagnosis difficult.
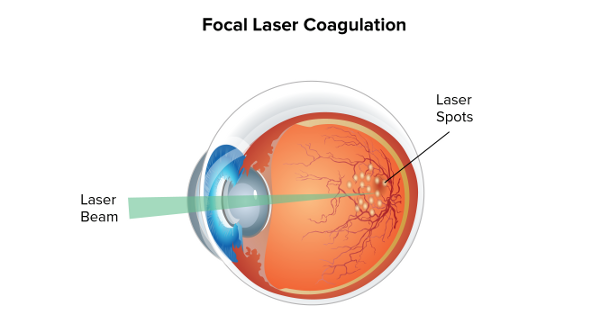
Once ocular melanoma is diagnosed, there are several options for treatment. Surgery may be used to remove all or part of the impacted eye, or radiation may be used to kill the cancer cells [7]. Laser therapy, either in the form of photocoagulation to damage the tumor’s blood supply or as thermotherapy to directly kill the cancer cells, is another potential treatment method [7]. However, the challenge is that in 50% of cases the cancer spreads to other sites in the body [1]. One patient, Allison Allred, has had the cancer metastasize to 6 different places in her body in spite of such measures as surgery to remove the cancerous eye [8]. Metastatic cancer is much more difficult to treat than primary cancer that has not yet spread. The 1-year survival rate for ocular melanoma patients whose cancer spreads to the liver is only 20% [1].
Researchers, including epidemiologists at the Alabama Department of Public Health, are trying to determine why so many people linked to Auburn and Huntersville have developed ocular melanoma. The group of cases is not yet being defined as a cancer cluster [2]. On first glance, this may seem perplexing – cancer clusters are characterized by a geographically defined, elevated caseload of a given type of cancer [2, 9]. However, classifying of a group of cancer cases as a genuine cluster is actually quite complicated. Many factors, such as genetic variation influencing cancer susceptibility, the time required for the cancer to emerge, and the plethora of carcinogens that individuals may be exposed to make it difficult to definitively link a group of cases to one common exposure [9]. It is fairly common for the cause to remain undetermined [9].
A previous report, released in June 2015 from the North Carolina Department of Health and Human Services, details the results of one investigation into the potential cancer cluster in Huntersville. The researchers determined that ocular melanoma cases diagnosed between the years 2009 and 2014 did not constitute a significantly above-average caseload, but they did point to excessive exposure to UV radiation as a risk factor for many of the patients included in the study [10]. No definitive cause was elucidated by the department’s work. Research on the Huntersville cases continued after the aforementioned June 2015 report, and not all findings have been published as of yet [11].
The story is rather different for the Auburn accumulation of ocular melanoma cases. While the diagnoses have been occurring since 1999, the trend seems to have just gained broad visibility this year. A CBS News investigation published in February of this year listed only 5 cases as Auburn affiliated whereas reports in May listed the more accurate number of at least 38 cases having a connection to Auburn [12, 1, 2]. The increase did not come from additional diagnoses of ocular melanoma between February and May; rather, the scope of the cases was simply not yet apparent in February. Advocacy by ocular melanoma patients, particularly by Ashley McCrary, appears to have assisted in unveiling the pattern. McCrary informed her doctors that some of her friends from Auburn University had previously been diagnosed with ocular melanoma and started a Facebook page asking for other ocular melanoma patients from Auburn University to step forward [8]. Her efforts identified additional Auburn University-affiliated ocular melanoma patients and contributed to the decision of her doctors at the Sidney Kimmel Cancer Center to study the group of cases further [8]. The Alabama Department of Public Health is also investigating the matter [1, 2].

Although the patients diagnosed with ocular melanoma may never find out what caused their plight, it is still critical to try to understand what led to these cases. Determining additional risk factors or definitive causes of ocular melanoma is a vital step toward prevention of this often deadly form of cancer. Funding is a necessary prerequisite for this research, so a group of patients inspired by the ALS Ice Bucket Challenge have banded together to initiate the Eye Patch Challenge. This challenge asks participants to wear an eye patch for a video, emphasize the importance of regular eye examinations, donate, and nominate someone to take on the challenge next [13]. In addition to raising money for ocular melanoma research, the organizers of the Eye Patch Challenge hope that it will result in increased awareness. The Ocular Melanoma Foundation has a related but distinct annual program called Eye Patch Day [14].
Some research on ocular melanoma is already being conducted around the country, including here at UC San Diego. Two principal investigators, Dr. Kang Zhang and Dr. Kun-liang Guan, have a grant from the NIH funding research into the molecular genetics of ocular melanoma. This ongoing project could assist the development of new treatments for ocular melanoma.

There are also measures that individuals can take to reduce their risk of ocular melanoma and to promote positive therapeutic outcomes. Eating a balanced diet to promote general health and wearing sunglasses to limit the amount of UV radiation that reaches your eyes are both measures recommended by the Ocular Melanoma Foundation [15]. Furthermore, one of the missions of the Eye Patch Challenge and of Eye Patch Day is to promote awareness of the importance of getting regular eye check-ups. The Ocular Melanoma Foundation states that annual eye exams, or at least an exam every other year, can allow ophthalmologists to diagnose ocular melanoma and other eye disorders earlier when they are easier to treat [15].
[hr gap=”0″]
Sources
- https://www.cnn.com/2018/05/01/health/ocular-melanoma-eye-cancer-bn/index.html
- https://www.npr.org/2018/05/04/608512592/doctors-stumped-by-rare-eye-cancer-cases-in-north-carolina-alabama
- https://www.aao.org/eye-health/diseases/what-is-ocular-melanoma
- https://www.aao.org/eye-health/diseases/ocular-melanoma-cause
- https://www.wcnc.com/article/news/investigators-release-eye-cancer-findings-in-huntersville/275-540363436
- https://www.aao.org/eye-health/diseases/ocular-melanoma-symptoms
- https://www.cancer.gov/types/eye/patient/intraocular-melanoma-treatment-pdq
- https://www.cbsnews.com/news/ocular-melanoma-eye-cancer-detected-two-groups-huntersville-north-carolina-auburn/
- https://www.cancer.org/cancer/cancer-causes/general-info/cancer-clusters.html
- http://epi.publichealth.nc.gov/oee/docs/OcularMelanomaInvestigationReport_June2015.pdf
- https://www.healthline.com/health-news/mysterious-clusters-of-eye-cancer-in-south-baffles-experts#6
- http://www.cbs42.com/news/cbs-42-investigates/cbs-42-investigates-rare-cancer-mystery-in-auburn/947521185
- http://www.wltz.com/2018/05/17/om-patients-launch-eye-patch-challenge-raise-awareness-funds-research/pic/108334/
- http://www.ocularmelanoma.org/eyepatch.htm
- http://www.ocularmelanoma.org/screening
