By Sharada Saraf | SQ Online Reporter | SQ Online (2016-2017)
________________________________________________________________________________________
With winter quarter in full swing, you might find yourself reflecting on your performance from last quarter. Perhaps you’re rewarding yourself on your successful time management with a well-earned burrito from Goody’s. Or maybe you’re cursing your unrelenting procrastination while continuing to procrastinate. Yet, as you take more challenging classes, you are required to improve your study habits in order to achieve your personal goals. Incidentally, this is the basis of what we have in common with viruses. Instead of attacking new course loads, however, viruses attempt to target and invade new hosts, often invading human cells.
A recent study led by scientists from the Scripps Research Institute found that the Ebola virus in particular was actively adapting during the peak of the epidemic from 2013 to 2016. One form of the devastating virus, called GP-A82V, had a genetic mutation that allowed it to more effectively target human cells. Consequently, that strain was found to have made up over 90 percent of infections during that time period.
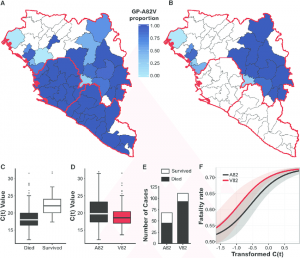
A team of Scripps scientists led by Dr. Kristian Andersen studied the Ebola virus using a sequence catalog of viral genomes created from over 1,400 known Ebola cases, and found the GP-A82V on Ebola’s glycoprotein, or outer protein. Because this glycoprotein is responsible for binding its receptor on host cells, mutations in this area often impact the virus’ ability to spread. This is the first time that a mutation has been found in the receptor of the virus since the first Ebola outbreak of 1976, so this study can explain why the virus had such a heightened infectivity rate on humans so suddenly, claiming the lives of over 11,000 people.
Further supporting this theory is the observation that GP-A82V emerged in the early stages of the epidemic, just before the exponential rise of Ebola cases. When scientists tested the GP-A82V mutation on different types of animal cells, they found that primate cells in particular were most likely to be infected. While the researchers still aren’t sure as to why this is, one hypothesis holds that the mutation modifies the amino acids in the Ebola virus receptor binding area, which allows the glycoprotein to better bind itself to human host cells, like two puzzle pieces fitting together. With large outbreaks of Ebola or other viruses, researchers think that these diseases can evolve to become more successful in a specific host.
The next step for Scripps scientists and their collaborators is to examine the relationship between infectivity and mortality rates in regards to viruses. These researchers hope to use their study to show that genome sequencing can allow scientists to respond more effectively to epidemics by modifying treatments to specific strains of viruses, thus reducing the number of tragic deaths that result from these epidemics.
[hr gap=”10″]
Sources:
http://www.scripps.edu/news/press/2016/20161103andersen.html

