By Julia Brown | UTS Staff Writer | SQ Online (2014-15)
Sleep, the bane of the average college student’s existence, might be a vital asset to those coming back from war. Often, soldiers returning from combat suffer some form of post-traumatic stress disorder (PTSD). The mental condition occurs primarily in those who have undergone tremendously terrifying or otherwise extremely undesirable situations and may take many forms, from severe anxiety to outbursts of aggression.5 One of the more common PTSD symptoms is difficulty sleeping, and while not much is known about the relationship between PTSD and sleep, a recent study from the UC San Diego School of Medicine and Veterans Affairs San Diego Health Care System reveals that quality sleep may increase the effectiveness of cognitive therapy as treatment for PTSD.
The study examined the effects of fear conditioning and its opposite, safety signal learning, on sleep.1 More specifically, the study examined
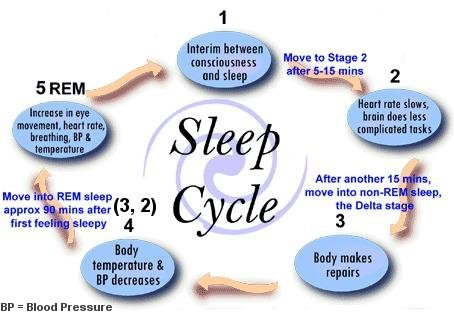
these effects with regard to rapid eye movement (REM) sleep stages, which are the portions of sleep cycles in which people have their most vivid dreams and experience related physiological symptoms, as shown in Figure 1 (left). Forty-two volunteers completed three days and nights of the study, in which they were subjected to various levels of electric shock combined with a corresponding visual cue.4 Cues associated with shocks were considered fear stimuli, whereas cues with no shock were known as “safety signals.” The researchers found that safety signal learning increased the quality of REM sleep, and the participants were better able to “distinguish threatening stimuli from safe stimuli the next day.”1
The “findings are not conclusive,” simply because of the relative lack of other studies regarding REM sleep and its relationship to PTSD.1 One potential path closer to understanding said relationship, the researchers propose, is “actively manipulat[ing] REM sleep to test the causal role of REM sleep in fear and safety learning.”4 If what the findings of this study imply about learning and memory consolidation is true, improving the quality of REM sleep in veterans might help ease their PTSD symptoms, and one way to improve said quality of sleep is via safety signal learning. While the implication is hopeful, the conditions might not be so simple. One reason for this lies in the habits that soldiers may develop or maintain as a result of their experiences in war.
After (and sometimes even before) returning from combat, many war veterans resort to alcohol or other drugs as mechanisms for coping with their PTSD symptoms, including sleeplessness.2 In the past, use of these substances, especially before going to sleep, has been shown to disrupt normal sleeping patterns,3 whether by correlation to a greater time spent trying to fall asleep, waking up several times, or decreased REM sleep.6
Due to the nature of their situation, PTSD-afflicted veterans are more likely than non-veterans to abuse these substances. Unfortunately, the
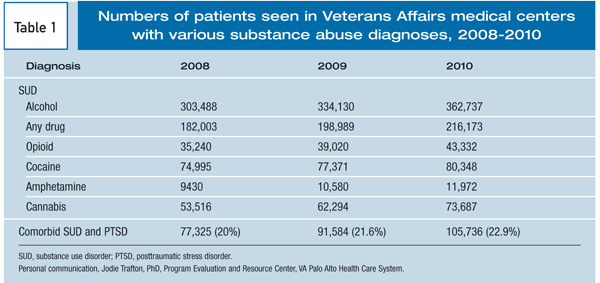
number of veterans diagnosed with substance abuse problems has increased over time, as shown in Figure 2 (right).
Thus, because of the relatively high rate of alcohol and drug use among veterans (as opposed to non-veterans), any PTSD treatment methods that might be derived from this study are further complicated by the methods by which these people try to handle their symptoms. This is not to say that this study is invalid; rather, it is to say that there exists a reason for more research to be done. If the results of this study are to have the widest effects possible, they should be coupled with increasingly effective methods of treating substance addictions.
[hr gap=”0″]
Sources:
- LaFee, Scott. “UC San Diego News Center.” Fear, Safety and the Role of Sleep in Human PTSD. University of California, San Diego, 26 Aug. 2014. Web. 27 Sept. 2014. <http://ucsdnews.ucsd.edu/pressrelease/fear_safety_and_the_role_of_sleep_in_human_ptsd>.
- “Veterans and Alcohol.” NCADD. Web. 27 Sept. 2014. <https://ncadd.org/learn-about-alcohol/seniors-vets-and-women/198-veterans-and-alcohol>.
- “External Factors That Influence Sleep.” Healthy Sleep. Harvard Medical School, 18 Dec. 2007. Web. 26 Sept. 2014. <http://healthysleep.med.harvard.edu/healthy/science/how/external-factors>.
- Marshall, Anisa J., Dean T. Acheson, Victoria B. Risbrough, Laura D. Straus, and Sean P.A. Drummond. “Fear Conditioning, Safety Learning, and Sleep in Humans.” The Journal of Neuroscience (n.d.): n. pag. 27 Aug. 2014. Web. 11 Oct. 2014.
- “Post-traumatic Stress Disorder (PTSD).” MayoClinic.org. Mayo Clinic, n.d. Web. 08 Oct. 2014. <http://www.mayoclinic.org/diseases-conditions/post-traumatic-stress-disorder/basics/symptoms/con-20022540>.
- Doghramji, Karl. “The Effects of Alcohol on Sleep.” Medscape.org. Medscape, 2005. Web. 11 Oct. 2014. <http://www.medscape.org/viewarticle/497982>.
Image Sources: